Home » Posts tagged 'Shibley Rahman' (Page 2)
Tag Archives: Shibley Rahman
Labour leadership pains: It’s not where you’ve come from, it’s where you’re going to
I must admit that I was taken aback when Gordon Brown quoted a former ‘successful’ Labour Prime Minister thus, “And, in Harold Wilson’s words, Labour is “a moral crusade or it is nothing”. I wasn’t so much amazed that Brown had decided to name drop a Labour Prime Minister who was well known for making policy up on the hoof, and possibly more into style than substance, but the fact that Brown had quoted one of Tony Benn’s favourite quotes ‘of Harold’. To understand the general approach of Jeremy Corbyn, you could do no worse possibly than to watch the film ‘Last Will and Testament’, where like Brown, Benn sets out the historical events which have inspired his quest for social justice. Brown’s penultimate line of conclusion was “And follow what Bevan called that decent instinct to do something that will help the lives of people most in need”, but I think that it is through looking that through this prism you can begin to understand the pain at the lack of efficacy of Labour’s so-called ‘opposition’. For example, Labour has never committed to reversing the destruction of the English legal aid system and the network of English law centres, claiming that such plans would not be possible given austerity. Austerity itself is the reason the NHS is being driven to do ‘more for less’, except the whole world and his dog knows that hospitals get by with the basic of staff on on-call cover, and idea of stretching out existing resources into a seven day way is laughable for most professionals within the service. It is therefore easy for me to understand the immediate popularity of Jeremy Corbyn; that he is defying the neoliberal doctrine, ‘there is no alternative’, with an alternative to austerity. This indeed is not an unelectable formula – look at Scotland (even though one can rightly moot whether SNP policies as actually legislated are particularly left wing). One can argue about whether Corbynomics will work, but the sheer defiance of the ‘there is no money tree’ with quantitative easing is worth raising an eyebrow at least. I have no idea whether Corbynomics is pro-inflationary, but then again no one else unless he or she happens to be an astrologer.
I went up to the Labour Party Conference in 2010 in Manchester. I got to Manchester Piccadilly precisely at the time that they were announcing the Labour Party’s new leader – who was Ed Miliband. Ed Miliband had defied the critics, and had come from nowhere to ‘seal the deal’. This was to much happiness of those who at that stage hated the Blairite wing of the party. I as such do not hate Blairism in the same way that I do not hate any corporates. I do not see Blairism as a social movement, but as a group of some extremely bright people but also some rather sanctimonious disparate people who can see no wrong in Tony Blair. I think many people use Chilcot as an excuse to hate Blair personally rather than a reason, but then again whether the UK went into war legally is a serious issue. I was greeted accidentally by Michael Meacher MP as I entered the ground floor of a pub in 2010 for the Socialist Societies meeting. I asked Michael if he was happy at Ed Miliband’s election: he said, “Not happy – ecstatic.” But he then added, “We’ve got our party back.” And I was to hear this phrase often during conference. And yet he struck me for the remainder of his term as leader that Ed Miliband was never a socialist, but a social democrat. That’s why I thought that the attacks of Red Ed were deeply fraudulent – but clearly not as ridiculous as the bacon butty jibes. When Gordon Brown referred continually to ‘Labour values’, this inevitably was a ‘fist pump’ moment for many, but it is essential to deconstruct whether Labour values, as espoused say by Keir Hardie, have been at the heart of the private finance initiative, where you end up paying for state assets through unconscionable loan agreements, or whether it is particularly Labour values to flog off the State’s infrastructure which you’ve invested in for decades. Lord Mandelson was one of the principal architects of the Royal Mail privatisation, so was it really possible for Labour to ‘oppose’ this when the time came? Is it a Labour value to remain relatively supine about the relative lack of nurses’ wages for many?
What has been incredible for me has been the sheer vitriol aimed at Jeremy Corbyn MP. Representing a different part of North London to the one I’m in, I ‘get’ his views on social housing. When you consider that the Mayor of London, currently Boris Johnson, does not have qualms about selling ‘new buys’ in Paris, making property prices unaffordable for residents of London, you get his point. When you also realise that without any forms of rent controls, landlords are regularly receiving state subsidy to provide accommodation at a huge profit, you see where Corbyn is coming from. However, there are substantial problems with Corbyn’s pitch in various areas, such as possibly exiting NATO. I remain unconvinced whether he really wants the Labour Party to stay in Europe. We all know his ‘friend and mentor’, as indeed he has called him himself, Tony Benn said ‘No Non Nein’ in the original EU referendum. Benn’s socialist reasoning was that he didn’t want everything to be run from unelected people in Brussels, which saw his logical reasoning go into an unholy alliance with the late Enoch Powell’s. But there is a substantial grouping within the Labour Party who do not see Europe as the great competitive nirvana that multinational corporates espousing free movement of capital and labour can do. They see it as a body which does not protect adequately workers’ rights. Corbyn may wish to take the EU negotiations from first principles with Labour. The attack on Labour during the Scottish referendum was that it was indistinguishable from the Tories – the scope for history repeating itself with the EU referendum is there too.
Harriet Harman MP was adamant that Labour should not be opposing for opposing’s sake, and that Labour had to have a moral drive and logic to its opposition. And yet it is Labour which perpetually gives the impression of being utterly toothless and taking it regardless. Its response to the Budget was pretty unmemorable, apart from Chris Leslie for all the wrong reasons. Andy Burnham MP somehow seems to arrived at losing from the clutches of victory, in no way helped by Harman’s stance on the Welfare Reform Bill. Burnham in ‘abstaining’ instead of giving an impression of firm opposition in the form of a ‘reasoned amendment’ which accounted for ‘collective responsibility’ looked instead as if he didn’t give a shit about the devastating effect of welfare cuts, including for the disabled community. Prof Germaine Greer in BBC’s Any Questions unsurprisingly therefore arrived at the conclusion that she expected HM’s ‘Loyal Opposition’ to oppose. There is clearly a feeling now that Labour should not oppose in a long-winged convoluted fashion. It is pretty hard to escape the conclusion that if you want to afford the NHS (not fraudulently articulated fraudulently in neoliberal language as ‘unsustainable’), you have to be willing to pay for it through general taxation. And yet Andy Burnham wants to set up a ‘Beveridge style Commission’ to arrive at this answer. His reasoning for this was presumably because his cherished National Health and Care Service, a great idea which would do much to make a ‘parity a reality’ (one of Burnham’s slogans before he railed against slogans), did not receive its democratic mandate. But there are vast swathes of NHS policy which seemingly do not operate on the basis of a democratic mandate, take for example the suggestion from McKinsey’s of £2 bn or so efficiency savings, or PFI. TTIP is yet another policy arm which, to give him credit, Burnham has been to Europe to oppose. Labour was not in government during the negotiations, but there is a general feeling that Labour did much to put in place the market infrastructure which made subsequent privatisation of NHS relatively easy.
(Cartoon by @BarkerCartoons)
As for Gordon Brown’s ‘Labour values’. where was tub thumbing Brown given the precipitous and disastrous privatisation of social care? It is a honest and settled view of many that social care funding is now on its knee, having not been ring fenced for the last few years. This simple fact makes Cameron’s view that England is the best place to live with dementia frankly delusional. A lot of reasoning behind Labour’s stance has been that it’s been ‘austerity lite’. Whilst socialism does need lots of money to succeed, or as the critics say ‘someone else’s money’, the state infrastructure does need a modicum of investment – even if the return of the investment is later to the City of London, as will inevitably occur when CrossRail or HS3 are flogged off. Tuition fees is another golden example of where a universal right to higher education has been marred with a requirement of an ability to pay. They say that somebody can easily land himself or herself a £60K debt bill at the end of university education, and I can well believe that. I am grateful for my university education, but equally I understand that university education is not the ‘be all and end all’ (for example we might wish to extend legal apprenticeships). I don’t like the A level system, as it’s my opinion it reflects more how well you’ve been taught than anything else, but there is so much mileage to be gained from my ‘I wouldn’t start from here’ arguments.
I do not happen to agree with the ‘savage’ attacks from the BBC in framing Gordon Brown’s speech as a devastating attack on Jeremy Corbyn MP. For example, Brown quoted Mandela in reference to the notion of the need for hope especially after years ‘in the wilderness’. My interpretation of what Brown was trying to say, albeit with a twang of ‘Don’t blame me if it all goes horribly wrong’, was that any Labour leader must receive the popular vote to get elected in the first place; but once elected it will require a huge effort from all sides to make Government work. I think this is particularly the case for Jeremy Corbyn. At one level, the popularity for him is not the same as left populism, it might be argued, and that the echo chamber Corbynmania and packed out lecture halls are not representative of the Labour voting public at large. We’ve been there before with a heightened sense of optimism, for example Milifandom. You don’t have to go far back in time to get constructive knowledge of polls which have been totally wrong – it could be all the ‘hard entryists’ into Labour do not vote for Corbyn at all, though I have no idea what a million Toby Youngs or Dan Hodges are like. There is a huge risk that Labour is about to enter an extended period of mockery, but you have to remember that Labour had relatively little hope of winning 2020 in any form anyway. Tony Blair is to blame in my opinion definitely for not having done the ‘succession planning’ properly; or you can argue that he is in fact an incredibly successful politician for having pulled the ladder up from underneath him. I think Blair has left in many areas a very formidable legacy as a social democrat, for example LBGT equality, public services reform, devolution, national minimum wage, but the essential problem with all of these policy planks is that we remain utterly clueless about the destination of travel. But the same can be said of Gaitskell or Wilson. But not Attlee – and therein lies some of the trouble. And as Nye Bevan said, “It’s not where you’ve come from, it’s where you’re going to” – or “If you remain in the middle of the road, you’re bound to get runover.”
“I dreamed a dream” – why the quest for a new leader cannot be merely a popularity contest
Instead of a complicated voting procedure, some have called for the Labour leadership to be decided by a popular one-off vote like ‘X factor’.
The candidates might be ‘dreaming the dream’, but are any of them the political equivalent of Susan Boyle? That is, a humble person from a modest background, with remarkable talents, with a unique offering. Someone who can click with the audience?
It is likely that Labour is throwing itself full speed into something it doesn’t actually need. That is, to choose a leader before it has chosen (or written) any of its policies. It would probably have been sensible to choose a ‘caretaker leader’ before asking people to choose the new leader.
Already, the search for a leader seems to have made certain assumptions. The leader has to have appeal to ‘voters’ rather than ‘people’. This market segmentation was last tried in Miliband’s hugely unsuccessful “35% strategy”. Again, one assumes the emphasis will be on ‘hardworking people’, and the rest.
In yesterday’s Question Panel, very succesfully chaired by Kevin Peel, who is undoubtedly a future successful Labour MP, a question came up which asked for which car Labour would be if it were a car. I suggested on Twitter, a “lemon car” – this is a car which is defective, with the back soldered onto the front, but with a lick of paint hoping that nobody notices. This was my analogy to Labour embracing the market into socialism, to make a new hybrid economy which is equally defective. A tweep remarked simply: “a bad one”.
The Question Time panel then were faced with the question how to stop the social media preaching only to the converted. None of the guests actually answered the question, but it was a good one. I felt this with the numerous “tweet storms”. Don’t get me wrong. They were hugely successful, and got various memes trending. But there were always a sense that there were there to make the activists feel happy, rather than reaching out to new voters.
But some people in Labour do have very strange ideas. Tristram Hunt MP, who may or may not be known to you as the Shadow Education Secretary, wanted to reach out to the granola buying voters in Waitrose (he didn’t actually say ‘granola’ but he did say ‘shoppers in Waitress’). This might have been Tristram Hunt saying the first thing that came into his head, as he offered a much more sensible answer on Question Time on another occasion.
The broad consensus is that Labour now has to be a “broad church” or a “big tent”; except one gets the impression that Len McCluskey is doing the proverbial in the tent. Labour’s problems are not simply a ‘Southern Discomfort’ as identified by the Fabian Society after the 2010 general election. The results indeed represent an ‘All Round Discomfort’, with voters to ‘the left of it’ in Scotland (going to SNP), and voters to ‘the right of it’ (going to the Tories everywhere but particularly in the South West), “stuck in the middle of you”. But there’s also the UKIP contingent in the North East who are not ‘taking a second look’ at Labour.
Labour wants now to have a ‘radical change’ akin to the Philip Gould ‘Unfinished revolution’ which gave birth to New Labour. Labour is unable to implement any of its policies, left or right, if it is not in power. Tony Blair was the last Labour leader actually to win a General Election; but he was also the one, for many, to take men into an illegal war allegedly.
But many still feel uneasy but what happened in the very recent past. Jon Cruddas seemed to spend ages commanding the development of a new prospectus, along with Ed Miliband’s various thought leaders. The prospectus was generally thought to be ‘good’ but, as Jessica Asato commented yesterday, “did not have winner stamped on it”.
With Ed Miliband’s Labour rejected by the electorate, various members have booked themselves into the radio and TV studios of England. They include Alan Milburn, Charles Clarke, Peter Mandelson, David Blunkett, and Alan Johnson. Yes, a group of “has beens”, or “also rans”, from New Labour, who were themselves ‘the future once’.
But in picking over Miliband’s political grave, they have provided the incorrect analysis. They have produced nostalgia over the word ‘aspiration’, presumably thinking of the white van driver Labour seems difficulty in tweeting to. But they all seem to miss the point – is it particularly aspirational to have introduced tuition fees, was it aspiration to or introduce the policy of NHS foundation trusts which meant that hospitals were seeking gongs ahead of an ability to deliver patient safety?
Labour I feel was rightly criticised for offering a good critique, but not offering the ‘sunny uplands’. The Conservatives, on the other hand, offered a ‘sunny uplands’ which was devoid of any truth. George Osborne missed the majority of his own self-set ‘targets’ in his last term of office. He has urged voters to ‘stick with the successful long term political plan’, and yet in a bravura of cognitive dissonance is about to present yet another ‘emergency budget’.
The lack of vision means that Labour gets fixated on the problems, albeit problems which do matter to many voters. To take as an example, Andy Burnham MP is keen not to let go of the ‘NHS is being privatised’ campaigning theme still for leadership, even though this received a hostile reception from the Tory press. There’s talk too about failing A&E targets for the 30th week in a row, et cetera. But the fundamental issue still remains – what does Labour wish to do about it? The Conservative Party really now are in a fix, having pledged not to put up taxes, but it really is in trouble in that it has no public mandate to increase taxes to fund public services. The Labour Party, on the other hand, could say that it wants to integrate finally health and social care.
Integration of health and social care is in the Conservative Party manifesto and probably is not going to happen. The repeal of the Human Rights Act, popular with Daily Mail readers, is on the other hand about to happen. And guess what? A leading political editor for the Daily Mail has just been appointed to run George Osborne’s communication strategy. Amazing.
Not even the Conservative Party were expecting to win the election outright, though they probably thought they were in a chance when it became obvious that the English electorate were indeed terrified of a Ed Miliband run government only supported by Nicola Sturgeon. It’s pretty likely the Conservatives were hoping that some of their pledges would be lost in political negotiation in a ‘likely hung parliament’. The English probably felt as comfortable about being run by the Scots, as, as we are led to believe, they were as comfortable as being run by the welsh Neil Kinnock.
But the man upon whom Ed Miliband waged war, Rupert Murdoch, was clearly a winner. Murdoch has helped to further the meme that ‘a political party only wins when it leads from the centre’, which has left many in shock knowing that ‘the centre’ has drifted progressively ‘to the right’. The meme may itself as successful as Ed Miliband’s “Britain only succeeds when its hardworking people succeeds”, which might be on a good day described as ‘aspirational’.
But how can hardworking people succeed? They might not be in abusive zero hour contracts. Or their cost of living might be good? This should sound familiar as it is. But furthermore there is nothing more aspirational for people in employment than securing employment rights. It is difficult to be aspirational when faced with overwhelming insecurities. In other words, whether or not you believe in ‘left wing’ or ‘right wing’ is a bit immaterial, but it’s perfectly possible to adopt a left wing narrative on aspiration, if you so desire. Aspiration is not simply about amassing material wealth; it is very much to do with furthering one’s own wellbeing.
Labour may be ‘dreaming the dream’, but there’s no Susan Boyle on the horizon, so to speak. I am not even sure that the current leadership candidates can ‘talk a good talk’, let alone ‘walk a good walk’. But history is certainly repeating itself, with the Tory supporters talking of ‘turmoil’ and ‘crisis’.
But it is indeed a crisis entirely of its own making. There is a curious strong sense of denial which continues to engulf Labour, which means that it cannot engage with opposing points of view. This explains why, despite its target of a million conversations, it seems more stuck in transmit mode and centralist, than wishing to learn.
Take for example the assumption that Scotland voted SNP because the Scots want another referendum soon and they are simply nationalist. I dare say that if the UK were to reject the renegotiated settlement of the EU that would trigger another referendum, but that surely is not the point.
Scottish voters did not in the majority vote SNP because they’re nationalist; but because they’re not in the ‘centre right’ ground – they’re quite socialist. And if you think about the SNP have in fact on the whole drifted to the ‘left’ – and a landslide to show for it.
The Liberal Democrats and UKIP should pledge to repeal the Health and Social Care Act
Ed Miliband, Andy Burnham, and the whole of Labour have pledged robustly that a direction to repeal the Health and Social Care Act (2012) will be made in the first Queen’s Speech of a new Labour Government.
It is said that David Cameron and Nigel Farage are to be issued with a joint challenge to declare that they will rule out any attempt to repeal the ban on foxhunting if they form a pact in the event of a hung parliament.
Evan Harris on 6 March 2012 identified the impact that the Lansley legislation would have to turbo-boost marketisation and privatisation of the NHS.
He warned Liberal Democrat colleagues not to touch it with a bargepole:
“It has no friends among even the non-party-political royal colleges, and has no mandate in those areas where it goes beyond the coalition agreement. The political impact will be to retoxify the Tory brand – which they are welcome to do, of course –, but also, by association, to damage the Lib Dems.”
The assurances given by Lord Clement Jones have turned out to be hollow:
“In putting down amendments, we have no hostility to competition as such, merely a desire to make use of the opportunities that the TFEU and European competition law offer member states to avoid the NHS being treated like a utility, such as gas and electricity.
Under the EU treaties, Article 106 of the Treaty on the Functioning of the European Union states:
“Undertakings entrusted with the operation of services of general economic interest … shall be subject to the rules contained in this Treaty, in particular to the rules on competition, insofar as the application of such rules does not obstruct the performance, in law or in fact, of the particular tasks assigned to them”.
Member states have certain discretion as to which services are services of general economic interest. By ensuring healthcare services for the purposes of the NHS are services of general economic interest and that the “task” of co-operation between services is “assigned” to the healthcare providers, it should be possible to provide some protection from less desirable aspects of competition law.”
This year saw Cambridgeshire and Peterborough NHS Foundation Trust awarding G4S Integrated Services a £3.9 million contract to provide domestic cleaning, portering and catering support across its property portfolio. The three year agreement, with the option to extend for a further year, will see G4S initially delivering services to 34 sites across Peterborough and Cambridgeshire, with further locations likely to be added in the future. Cleaning will be provided across the contract, with additional portering services and catering support at some specific sites.
Privatisation does not require a complicated definition. It’s simply the transfer of public sector resources into the private sector. Even the late Sir Keith Joseph, widely thought to be “brilliant” by the late Margaret Thatcher herself, and who was thought to be the principal “architect” of Thatcherism, ended up trying to keep afloat businesses in the public sector rather than privatise them. This was during his time as Secretary of State for Trade and Industry.
There is generally a feeling that the Coalition government, a joint enterprise between the Conservatives and the Liberal Democrats, went much further in privatising the NHS than the Thatcher government even dared to. And the worst aspect of this was there was absolutely no inkling that this would happen. There was no mention of this even in the Coalition Agreement of 2010.
There is no official policy by UKIP on the NHS yet.
This is absolutely staggering. The late Tony Benn used himself to warn people against voting for people who are ‘false prophets’. UKIP seem alarmingly reluctant to acknowledge the number of people from black asian minority ethic background who actually work for the NHS and bring value to it everyday.
It is now felt that there is quite a high chance of a ‘hung parliament’, although Labour activists are desperate to fight for a Labour government at Westminster with a healthy majority. It appears that the mainstream right-wing press have given up the ghost, in the form of David Cameron.
It is curious why the Conservative Party haven’t ditched their leader, like they did famously in 2010, but the most parsimonious explanation is that it would make sense to find a new leader after the expected catastrophe of the 2015 election. Ditching Cameron now might mean that they would have to ditch a new leader further in 2015. Besides, the Conservatives and Liberal Democrats have become a tried and tested product as far as the City are concerned.
The current Government, and people who sail with her such as BoJo, have fiercely defending the City’s interests in Europe as far as banker bonuses are concerned. They have resisted the ‘Mansion Tax’, which is widely thought to be introduced by Ed Balls as Chancellor in the first Budget of a Labour Government, as a windfall tax to produce a cash injection into the NHS. Furthermore, the City still has lucrative contracts in the form of the private finance initiative which have yet to be renegotiated properly from this Government; and also they have been very successful in promoting social impact bonds, the PFI equivalent for social enterprises, with the current Government which has used mutualisation to Trojan horse rent seeking in response to Mid Staffs.
Certain dividing lines have now got to be laid for the sake of the public good.
I feel that it is essential that David Cameron, Nick Clegg, and Nigel Farage are to be issued with a joint challenge to declare that they will rule out any attempt to resist the repeal of the Health and Social Care Act (2012).
Nigel Farage, for all his faux socialist credentials, seems unseen to resist formally the privatisation of the NHS; in fact his henchmen over the years have prided themselves on the ‘efficiency’ of the private sector, despite the growing allegations of fraud and inefficiency from the outsourcing companies used by the current government to deliver the smaller State.
Nick Clegg not only has a PR problem; he has a major issue with the content of what the Liberal Democrats stand for. It is widely known that there is discontent about his party’s ‘differentiation’ policy, which has seen the Tories and the Liberal Democrats telling the voters why each other party is clearly unfit for government. The charge sheet against the Liberal Democrats, including a weak economy (not enough till receipts from income tax to fund public services), demolition of legal aid, privatisation of NHS, misery for a mass of disabled citizens through botched welfare reforms, is substantial.
As a minority party, the Liberal Democrats would be asked to repeal the Health and Social Care Act (2012) which is possible but simply weird. It is clear that the Liberal Democrats, Conservatives and UKIP are clearly capable of running the NHS into the ground.
A lot of energy was put into fighting the Liberal Democrats on the toxic firestorm hospital closure clause, clause 119, which the Liberal Democrats were instrumental in protecting. Norman Lamb, for all his soothing words, has been the Minister of State in office while social care has imploded; the social care budget has not been ring fenced, coincidentally, since 2010.
There was a popular joke on Twitter this year that turkeys joked, “It’s like humans voting for UKIP”.
David Cameron, if he is still leader in 2015, or whoever is in charge of that toxic brand, will clearly be in no position to repeal the Health and Social Care Act (2012). The least worst option is that the Liberal Democrats and UKIP should pledge not to resist the repeal of the Health and Social Care Act (“Act”), but the hope is that a strong Labour government will have renewed vigour in assessing the political weather. Even better, they should pledge to repeal the Act.
That is, the component of the private sector in the mixed health and care economy has gone way too far. The health and care sectors should never be run anywhere for the benefit for shareholders offering care in 15 minute slots or below the minimum wage. The health and care sectors should not be so fragmented as they are now. People should be collaborating with each other to offer excellent clinical care, not competing with each other.
The vote is the most critical weapon of influence any of us has. Even more than ever, it is vital that it is used wisely.
Reasons to be cheerful – my review of 2014
There were many reasons to be cheerful this year for me. One of them was going down at the invitation of Lisa Rodrigues (@lisasaysthis) for Prof Sube Banerjee’s inaugural lecture as Chair of Dementia at Brighton and Sussex Medical School.
Reasons to be cheerful
Sube called his lecture, a timely view on where we’ve got up to in English dementia policy, “reasons to be cheerful”.
Kate
Kate (@KateSwaffer) is a world class advocate for people living with dementia.
I have found Kate’s work on stigma and language particularly interesting. Kate is Chair Elect of Dementia Alliance International (@DementiaAllianc), and I expect this group, consisting in the vast majority of people living well with dementia, to be extremely influential in 2015. As this group becomes more influential, I am sure it will attract more scrutiny, and it will be necessary both to manage people’s expectations and not be unduly swayed by externalities.
The University of Wollongong (@UOW) is where Kate did her Masters of Science degree in dementia care. I only received a Commendation for my Master of Law, but that was in commercial and corporate law, and not really my strongest love. For Kate to receive a Distinction is no less than Kate deserves, and I was genuinely utterly thrilled for her.
Chris and Jayne
I tried to get out more this year, fuelled by seeing friends Chris Roberts (@mason4233) and Jayne Goodrick (@JayneGoodrick). Louise and Rachel from the Dementia Action Alliance Carers Call to Action (@DAACarers) have worked amazingly hard, and I have nothing but the utmost respect for this arm of English policy. Here’s a picture of me, Chris, Sally (@nursemaiden) and Ken Clasper (@ken_kenc) at the Methodist Central Hall in Westminster.
I do strongly believe that ‘experts’ are a potentially false concept in dementia. I certainly don’t believe in experts by longevity – people who’ve professionally been studying dementias for ages. I do agree with Chris though – people living with dementia do become experts in their own experiences at their particular times. We all can learn from this.
Here’s Chris holding the Dementia Alliance International flyer. This was in a crowded foyer during the conference. I am not sure what we were doing at that precise second. I reckon I might have been panicking about the poster session on my findings of the use of language in the G8 summit. That poster session was very enjoyable for me, as I got a chance to chat with Prof Mary Marshall whose influence on design and dementia has been enormous at Stirling. Mary remembered me from a workshop I attended in Notting Hill once. And I remember her. She spoke with me for ages, when she had no need to at all.
Dementia policy in England and Scotland
I thought this was a parody of a Monty Python sketch until one of my bright Twitter followers advised me it was a parody of the Two Ronnies sketch. That’ll learn me. Anyway, here I am with Chris and Tim Lloyd Yeates (@alivetim) whom I am confident to report is one of the most polite and well mannered persons I have ever met in my life.
Ultimately, I have limits to my understanding of dementia, having not lived with dementia myself to my knowledge, and definitely not been involved in a family caregiving way. I am all the time mindful there is close to a million unpaid family caregivers in the UK, who are the backbone of dementia policy. They are central to care and support. Sally Marciano is a very experienced nurse, but also knows from the closest of family connections how dementia can affect someone. Prof Alistair Burns (@ABurns1907), the national clinical lead for dementia, often remarks that when a diagnosis of dementia is disclosed, it’s not only given to the person with dementia, but to his or her friends and family. This, I feel, is absolutely true.
I first met Toby Williamson from the Mental Health Foundation (@MHF_tweets) when he chaired a groupthink session in one of the fringe meetings of the Alzheimer’s Europe conference in Glasgow. We were discussing stigma in dementia, and thinking of possible strategies for overcoming stigma. Toby is at the Mental Health Foundation, and I find him extremely interesting to talk with. He shares a number of policy interests with me, namely human rights, equality and personal budgets. I name dropped Toby in a comment on Prof Julian Hughes’ excellent presentation on ethics at the annual meeting of the Dementia Action Alliance.
Thanks to Sam (@yeweestoater) for her unending support. I really value this – and I had a great time when I met Sam for the first time at the Beardmore Hotel in Glasgow earlier this year, for the clinical research network day hosted by Scotland.
I was invited by Norman Macnamara (@norrms) to a talk on global positioning systems and people living well with dementia. As it happened, I got lost on the way back to the lift of the Queen Elizabeth II conference centre, and Norman was very helpful! The Purple Angels continue to be an enthusiastic force of people raising awareness of issues to do with dementia.
I have decided I am no longer going to take photos on my digital SLR camera, as something always go wrong on them. Here’s a photo of Suzy (@suzysopenheart) and Jayne not taken on my iPad as it should’ve been (like Tommy Dunne (@tommytommytee18), I adore my iPad).
I was really pleased that Lucy Jane Masters (@lucyjmarsters) was able to make it to my book launch of ‘Living well with dementia’ earlier this year.
It was great to see Marian there (@mariannaidoo). Also, I really appreciate Beth (@BethyB1886), Dr Peter Gordon (@peterDRLOW) and Margaret Kilby (@mkilll) making it too.
Lucy is a specialist nurse in dementia, and also studying at the Brighton and Sussex Medical School. Like me, Lucy shares a passion for the positive rôle specialist nurses can play in proactive case management in dementia, which I anticipate will be an important service provision change innovation shortly.
Travelling back to Glasgow was highly emotional for me; so was meeting people who’ve become a big part of life through Twitter. You certainly can’t fault Tommy Whitelaw (@tommyNTour) for the sheer dedication he has shown to raising awareness of lending a hand of support for caregivers. Besides, he’s a Glaswegian, and given that I was born in Glasgow in 1974, Glasgow is a special part of my own personal life.
There are people I met in 2014 – and I wish they’d come into my life earlier, really. I was always aware of the huge amount of work Agnes Houston in the Scottish Dementia Working Group was doing as well as Donna. It was only until I saw Agnes (@Agnes_Houston) and Donna whizzing around in the Alzheimer’s Europe (@AlzheimerEurope) conference in Glasgow that the penny finally dropped.
I don’t think I ever met Tommy Dunne until this year. Meeting Tommy and Joyce were definitely highlights of my year – and I think Suzy Webster is genuinely fantastic too. With them, there’s no bullshit at all. They exhibit kindness. They are not distracted by others – their focus and attention is a clear indication of their dignity and the amount of respect they command. I think some of the happiest times I had in total in 2014 were through the Dementia Action Alliance Carers Call to Action (@Dementia_Action; @DAACarers). They’re the sort of occasions where you do genuinely feel you’ve known people for ages – like weddings without any of the family traumas!
Twitter can bring with it some degree of mystique. But a general enduring trend of mine was that the people I met in real life were invariably even more impressive than how I knew them from Twitter. One clear example of this was Darren (@mrdarrengormley). I think I share attitudes and values with Darren. Darren really ‘gets it’. A real privilege to know – I’ve got a lot of time for Darren.
Charmaine
To say Charmaine (@charbhardy) is ‘strong’ would be to do Charmaine a disservice. I am completely in awe of how Charmaine doesn’t ‘complain’. Charmaine thinks she’s doing her best, but she’s doing infinitely more than that. I am extremely grateful for the time I had this year in going to Robertsbridge and seeing for my own eyes the garden that Charmaine works so hard on. And I am proud of everything Charmaine does. I am proud of her community. Her friends adore her (look at the bunch I met for example at the Ostrich and Tony especially). I loved meeting G who spontaneously showed me his PhD thesis from around the time when I was born (I was born in 1974). This photo of Charmaine and me was taken at University College London, where completely thanks to Charmaine I was able to attend a support group for carers of people with frontotemporal dementia. There, I had a long chat with Katy Judd. It was great to catch up with Katy, whom I remember working with at the National Hospital for Neurology and Neurology, at Queen Square, more than a decade ago. Prof Martin Rossor (@martinrossor), whom I think is wonderful, was the head of the clinical firm.
I’ve learnt a huge amount from the support groups this year. It also reminds me what an enormous privilege it is to know something about dementias in a professional and academic capacity, and what an honour it is to use this knowledge for the public good.
I’d love to go to the Ostrich in Robertsbridge some time in 2015 for a holiday; not least as it will give me an excuse to see Charmaine G and family.
The international forum
Before I got a chance to finish my sentence, ‘My name is…‘, Marc Wortmann (@marcwort), CEO of Alzheimer’s Disease International (@AlzDisInt), explained to me that he knew ‘exactly who (I am)’. I had a chance to thank Marc twice this year for the work of the ADI – once for the work on national strategies in dementia, and one for his report in which the ADI recommended avoidance of the word “institutionalisation”.
Helga in many ways is larger than life. Helga Rohra (@ContactHelga) just beams encouragement, drive, wisdom, leadership, principles, justice, realism, and charisma. A real joy to spend any time with. Here’s us in Glasgow.
Prof Facundo Manes (@manesf) was in the same research lab as me at Cambridge. He is one of the world experts in frontotemporal dementia now. I have extremely fond memories of his friendship at Cambridge, and he has become a lifelong friend. He is a ‘proper neurologst’, and has a huge amount of common sense as well as a real talent for research. I love his attitude to life, and the fact that he is so clearly very bright. He has taken the field of decision making in dementia into parts I could have only dreamt of, and of course I am eternally grateful for that. Facundo, as well as being a Professor at the University of Favorolo in Buenos Aires, leads at INECO – a huge tour de force in cognitive neurology and cognitive neuroscience in South America; and he is Co Chair of the research division of dementia, aphasia and other cognitive disorders for the World Federation of Neurology.
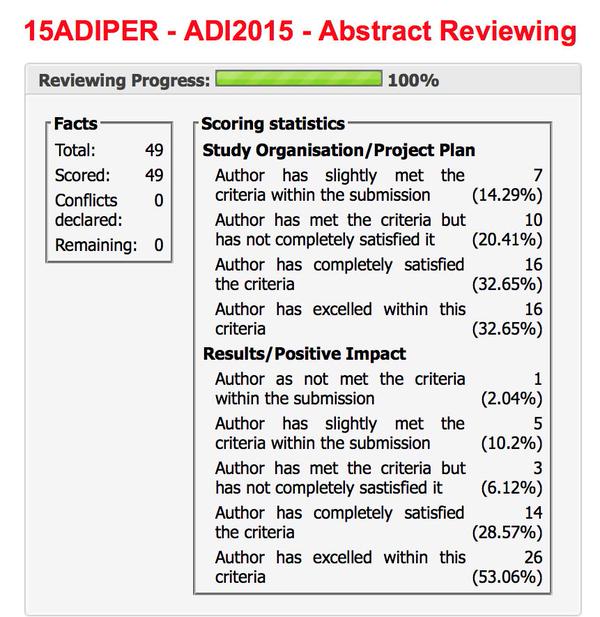
This year, I got put onto the International Advisory Board of the ADI conference to be held in Perth, Australia, this year. I really enjoyed reviewing about fifty abstracts mainly on stigma, younger onset dementia and dementia friendly communities. I look forward to these being presented, when I attend in person next year.
The law
One of the biggest honours I had this year was being asked onto the Board of Governors of the BPP Students’ Association. Prof Carl Lygo (@carllygo), Professor of Law, and CEO of BPP, has been of massive support to me personally. He’s supported me through the stormiest of weather. Also, Shahban Aziz (@ShahbanAziz), CEO of the BPP Students Association, has become a true friend of mine. I get enormously proud of them both whenever I see them in real life, or on Twitter.
In one part of my life, I thank enormously for the happy times I’ve had at BPP Law School. I not only studied for my ‘graduate diploma in law’ (and bachelor of law), but I also did my legal practice course there. This was via brief detour of doing my MBA at BPP Business School and my Master of Law at the University of Law. BPP has been a massive part of my professional and personal rehabilitation. Now, my understanding of business strategy and law make complete sense.
Here I am with Shaun (@DiasShaun) and Shahban.
I had the pleasure of talking to Gary at great length this year twice. Our conversations ranged from conflicts of interest to conspiracy theories. I think it’s fair to say I have met few people as thoughtful or as intellectually versatile as Gary Slapper (@garyslapper). We share very similar values. I am looking forward enormously to his new edition of ‘English legal system’, which reminds me of the second love of my life – the legal profession.

NHS
I have enormous respect for Prof Wendy Savage (@wdsavage). Wendy Savage and I share not only a passion for the NHS, although Wendy’s campaigning is in altogether different level to mine (being far superior). And Wendy, I suspect, shares similar feelings about the medical regulator, the General Medical Council, as me.
This year saw me trying to get out and about a bit more. I met Sharon (@SharonAvraham) outside the Harold Wilson room for a meeting which Jos Bell (@jos21) had brilliantly organised. Jos has worked so hard as Chair for the independent Socialist Health Association London division this year. Jos has also been a real rock of support this year, which has been tough for me. I am inevitably eternally grateful for this.
I saw Andy Slaughter (@hammersmithandy) speak for the first time in Portcullis House. I am of course fully aware of the West London hospital reconfiguration, and I thank Andy enormously for campaigning on this issue. I am also grateful for Andy’s lead against that nasty Legal Aid and Sentencing and Punishment of Offenders Act (2012) which saw legal aid being throttled. I am a firm believer in access to law and justice, as well as access to medicine. Of course I am mindful that Sadiq Khan, currently the Shadow Justice Secretary (@sadiqkhan), will have a difficult year ahead.
For the first and only time this year, I had an amazing smoothie and cheeseboard selection in the restaurant of the National Gallery. Like the late Baroness Thatcher, I have developed a habit of turning up to everything early. I turned up to the event in Trafalgar Square to support the NHS early. Jos knew I would. I had a great time, though.
A poor start
The very beginning of my life I don’t feel was a poor start.
I am Scottish. I went back to Glasgow twice this year in fact.
Glasgow is where I was born in June 1974.
Undeniably I feel I’ve come a long way since that I day I had an epileptic seizure at the Royal Free Hospital due to bacterial meningitis in 2007. Things got worse when I had a cardiac arrest, and then had six weeks in a coma. While I am physically disabled now, I am happy of course that I have been in recovery from severe alcoholism for about seven and a half years now. I feel strongly that anything can happen to anyone at any time.
GMC
I went up to Manchester several times in 2014 to see the GMC – my meeting with them was adjourned the first time around.
I ended up, therefore, contemplating in Starbucks.
With the free Wifi, it was like being on holiday.
It was amazing to meet @kyrakee who found me there. Kylie had just hopped off a tram, perhaps having worked out the clues from my cryptic Twitter clues?
I know this Starbucks now, like the Arnedale Centre, like the back of my hand
2014 was an opportunity to apologise to the medical profession which I strongly feel that I had let down previously. My late father amongst many others would have wanted me to have made this apology to the GMC (@GMCUK).
It was a massive honour to be put back onto the GMC register. I don’t think I have ever been happier. To be put on the UK register having lost the opportunity to be there is a massive deal. The GMC oppose all restoration requests not because they’re fundamentally difficult; but because the burden of proof must be on the applicant to prove that they can fulfil their duty of patient safety. There is therefore a necessarily high threshold for this, and now that I am in recovery, I don’t underestimate the enormous privilege to be regulated by both the medical and legal professions.
Martin Rathfelder (@SocialistHealth) took great care of me in my numerous visits to the GMC in Manchester this year. I have very happy memories of the numerous Chinese restaurants we frequented too. Martin was a crucial component in me trying to think positively about the whole experience. Manchester, after all, had been a very sad place for me and my father back in 2006. On a different note, I currently enjoy being on the ‘central council’ of the Socialist Health Association.
I am completely in awe of the GMC. I would say that, wouldn’t I?
Happiness at last
All these life experiences encourage me to try to take life easy when I can. Like a Koala, I can present #KoalaKlaws. I can even, if pushed, go for the #KoalaKill. I therefore have natural affinity to the Koala.
The man on the right of course needs absolutely no introduction. I think it’d be impossible for the English dementia policy to be universally liked by everyone. That I say not as means of an excuse, but because I am genuinely in admiration of how Prof Alistair Burns has served as the clinical lead for England. I met for the first time this year Alistair (here at the DAA Carers meeting at Smith Square, Westminster). I also met Sally Greengross (the Baroness Sally Greengross) for the first time this year. Sally’s the Chair of the All Party Parliamentary Group for dementia. I promised Sally in fact that I would include a chapter on arts, music and creativity in my next book. I like Sally would like to include some of the positives too in the narrative, and looking into this for Sally was a huge delight.
Next year will be a gruelling one. The last few years have not adequately safeguarded against causing misery for disabled citizens. Legal aid was murdered. Criminal barristers were in uproar. The NHS saw a piece of legislation which imposed a heavy penalty for the first time for NHS contracts not put out to competitive tender in all cases other than a sole bidder. The record waits for A&E were a disgrace for the operational management of the NHS in England. We now have a situation where it is difficult sometimes to discharge people in a timely fashion to social care. Bringing together health and care next year, if there is a majority Labour government in the UK, as “whole person care”. The repeal of the Health and Social Care Act (2012) which turbo-boosted the privatisation of the NHS, defined as the transfer of resources from the public to private sector, is now desperately needed. I wish Andy Burnham MP (@andyburnhammp) well. I sincerely hope he can start work as Secretary of State for Health and Care in 2015.
Conferences: a necessary evil?
I really didn’t know what to expect in the Alzheimer Europe conference in Glasgow. I must say that people with dementia and carers were certainly not involved in any tokenistic way. I was happy to be there. Thanks to all at Alzheimer Europe for such a brilliantly run conference; including the work done by Gladwys and Jean (@JeanGeorgeAE).
The conference brought me back to my academic roots – which is no bad thing.
As I grew in confidence this year, not just personally, but also in my opinion of the national train service providers and the London termini, I wanted to travel to conferences about dementia more. As the year progressed, my attitude changed from conferences wanting to sell you something, to conferences being happy places where you shared knowledge and experiences. Besides, they for me became happy places for me. Here’s James Murray-White (@sky_larking) and Chris at the Future Inn, Bristol, just shortly before our day hosted by Alzheimer’s BRACE (@AlzheimersBRACE).
Tommy Dunne and Chris Roberts were sat right at the front of my talk in Manchester. The turnout wasn’t massive, but it meant a lot to me that they were there. There was also somebody in the front row who was very nice to me; his mother had just been diagnosed with a dementia. To make a small difference to just one person means a lot to me. I’ve also felt this about ‘Dementia Friends’ (@DementiaFriends) – it’s not the quantity of the actions, it’s the quality.
Getting a chance to fill a void in print about living well with dementia meant a lot to me this year.
I straddle currently two professions, but I’ve been attending out of support (but not participating in, due to my disability) the legal aid walk for the last few years. Thanks so much to Bob and Natalia who invite me every year. I volunteered once pro bono in the North Kensington Law Centre, the oldest law centre in England, in welfare benefits. I had a brilliant time, and I would strongly recommend this type of work to any law student.
My books
This was a bit of sneaky product placement for my book, of course.
I was totally amazed to see my book in print. I dedicated my book ‘Living well with dementia’ to my late father, but of course without both of my parents this book would’ve been impossible.
Thanks to Prof John Hodges in NeuRA, previously Chair of Behavioural Neurology at the University of Cambridge, for the support he’s given me for my first book ‘Living well with dementia’ (where he indeed kindly wrote a Foreword), and also for my second book ‘Living better with dementia’.

I admire Alistair’s energy, so it was extremely nice to receive this from Prof Burns earlier this year.
Serenity
Above all, I was reminded from Truthful Kindness (@truthfulkindnes) this year not to worry about things which were clearly out of my control. This mantra, the “Serenity Prayer”, is how we conclude each meeting for people who’ve had alcohol problems. There comes a time when some people, having successfully survived a period of abstinence, go into a period of recovery. That’s when you get used to life in the absence of alcohol, and it’s normal. You don’t get cravings – you don’t notice alcohol – you can go into pubs without it even being an issue. So if things don’t go my way, invariably out of my control, I don’t fret about it any more.
Thank you for making my year such a happy one.
Why I do “Dementia Friends”
Let me introduce to you to “Dementia Friends” (details here).
The aim is for you to learn some fundamental information about what dementia is, so you understand it better than you would’ve done otherwise.
Dementia is caused by diseases of the brain; it can affect any thinking depending on what part of the brain is affected.
It’s not a normal part of ageing; it’s important to live well with dementia.
There’s much more to a person that the dementia.
I’d like to say something which may surprise you, depending on how well you know me.
I don’t really like the term ‘dementia friendly communities’. I totally ‘get’ it is well meant, embracing the concept that people living with dementia can go out in their communities at large, talk to people, go shopping, and lead a happy life.
But there are problems with the concept. I think it ignores the fact there are so many different causes of dementia, each with different ways in which they affect a person’s life. These dementias can progress at different speeds too.
I’m also worried about inadvertently creating division. There are enough divisions in society, e.g. rich vs poor, disabled vs non disabled, sick v well, for example.
I worry about the issue that to be dementia friendly you can immediately recognise disability. I’ve always had to bite my touch when people claim you can easily spot dementia in the community, so much so young schoolchildren can spot dementia even when experienced GPs cannot.
Dementia, like all other disabilities, can be invisible.
The term ‘dementia friendly community’ poses the same issues in principle as ‘gay friendly community’, therefore, one could argue.
Nonetheless, I feel the starting point policy-wise is that there is a huge amount of public ignorance about the dementias. The media have been notorious at misrepresenting dementia; even the term ‘epidemic’ is problematic, whatever the exact truth about numbers and definition, given that there are some people who believe that the dementias are essentially contagious.
I regularly ask London cab drivers if they’ve heard of dementia. Invariably, after saying ‘yes’, those cab drivers then can’t tell me much about dementia. These are generally well informed individuals, however. They readily admit they wish they knew more.
For me, it’s easy to underestimate what people know about dementia. I did a medical junior job at the National Hospital for Neurology and Neurosurgery in it. I also did my Ph.D. in it.
But I am in no way an expert.
One of my best friends, Chris Roberts, living with a mixed dementia of Alzheimer’s disease and vascular dementia, is a Dementia Friends Champion. He says, if he is an expert, he is an expert in his own dementia at this particular time.
Chris is on the left of the picture above; Jayne on the right. The “thing” in the middle, by the way, is a “selfie stick”, currently all the rage in England.
Thanks to the audio visual unit at BPP Law School for their helping me for my Dementia Friends sessions.
Here’s a short excerpt of the Dementia Friends information session we gave on 4 December 2014, together with Jayne Goodrick.
Our details are here.
It shouldn’t be the case that people who’ve been given a diagnosis of dementia feel somewhat frightened to tell their friends or family. We know loneliness is a big problem for many who’ve received a diagnosis of dementia in England.
I love doing ‘Dementia Friends’.
We never ‘force’ our Dementia Friends infocards and badges onto people!
I came to the programme with the same cynicism as many, wondering what was ‘in it’ for the charity involved in implementing it. I am genuinely worried about lack of diversity in the dementia charity sector, and potential abuse by one or two key providers of ‘dementia services’.
I also came to the programme with concerns about whether the messages or activities of Dementia Friends would be accurate.
I am generally very happy with the messages which Dementia Friends gives out, and the feedback has been overall very positive. No initiative is perfect by any means, and I think ‘Dementia Friends’ is as good a national programme, for what it does, as it could be. It was a major proposal from the 2009 English dementia strategy, entitled ‘Living well with dementia’.
The anonymous feedback we received from our December session was very positive.
The questions I regularly receive at my sessions are much harder than the ones I receive at international conferences on dementia. Such questions have included, “How can we promote the dignity of a person living with dementia?”
I think though, overall, the “Dementia Friends” initiative has succeeded.
Detailed analysis will see whether it has indeed been successful in turning ‘understanding’ into ‘action’. But I think there are currently about 600000 Dementia Friends at the time of writing is a major triumph.
Please book yourself into a Dementia Friends information session to decide for yourself. My next session is at BPP Law School in Holborn, London, on January 15th 2015. Details are here.
Another 5 years of David Cameron? I really hope not.

What is most intriguing in the in-depth analysis of Ed Miliband as Prime Minister is that most people I know would rather emigrate from the UK rather than to face another five years of David Cameron.
David Cameron has presided over an unbelievable mess in welfare benefits. I’ve lost count of people including myself who suddenly had their welfare benefits stopped (in my case disability living allowance due to physical disability), who just ‘fell off’ the benefits register. I had to have two appeals, and then go to a tribunal, before I was restored to the benefit I had received previously. And in the meantime there had been absolutely no improvement in my disability symptoms.
David Cameron has presided over an economy which works well for the very wealthy – but this is a dangerous time to be vulnerable. It is sheer bare faced cheek to claim the economy is healthy when it can’t muster enough tax receipts to keep public services going. A record number of people in employment, with a growing population in the UK, is short shrift for a society which cannot pay benefits in a timely manner such that a record number of people has to go to food banks. This is precisely what you get when you a bargain basement low wage economy, fuelled by zero hour contracts, with slashing of employment rights.
The Conservative narrative is a highly fraudulent one. Shortly before Lehman Brothers crashed, George Osborne had been boasting about how he would match Labour on spending commitments. So far from giving keys back to the driver who crashed the car, Osborne was the co-driver. Osborne wrote in ebullient terms about the deregulated Iceland – the one which crashed big time. It’s simply a pack of lies, needed to produce a malnourished State of public services, whereas corporates still get their cushy state handouts – such as proceeds from the privatisation of Royal Mail. This time, the Liberal Democrats, under Nick Clegg and Danny Alexander, have been first in the queue chanting repetitively their pack of lies.
David Cameron’s cardinal sin was never to mention the devastating £3 billion reorganisation of the NHS. This four hundred page piece of law, only made possible with the Liberal Democrats on the accelerator pedal not the brake, did not have a single clause on patient safety (apart from abolition of the National Patient Safety Agency). It was the wrong piece of law at the wrong time. With social care on its knees, it did nothing to make the health and care systems fit for purpose. Hospitals simply cannot discharge NHS patients in a timely fashion to social care currently. Add on top of this the chaos in A&E waits, it’s now a case that individuals cannot both enter hospital and cannot leave hospital. The NHS simply could not cope with another five months of this utter mess, let alone another five years under David Cameron.
Cameron and Hunt have presided over a disastrous NHS. How dare they.
But the legislation was not a waste of time for the people who have been behind this Government every step of the way. Lurking in the shadows of ‘The Big Society’ are the big private equity backers. They’re the ones who have controlling stakes in private finance initiative hospitals which they can slept a profit. Eye watering contracts of NHS services are being flogged off to the private sector. Even the late Harold Macmillan, a previous Tory prime minister, resented the selling off of the ‘nation’s silver’ under the prime successor, Margaret Thatcher. Privatisation is simply transfer of resources from the public sector to the private sector. You’d have to be an idiot not to understand that.
Somebody who is far from an idiot, Oliver Letwin, has explained the critical rôle of outsourcing of services (source here).
Just in case there is a hung parliament it’s become vital to think who could prop up another failed Tory administration. Vote for Alex Salmond or Nick Clegg at your peril.
Is it too little too late?
We found out this morning from Dave West from an article in the HSJ that HM Treasury has agreed an unannounced £740m increase to the health revenue budget for the current financial year.
Since mainstream parties agreed to sign up to ‘efficiency savings’, a euphemism for making cuts in budgets, NHS Trusts all over the land have been trying to reconcile PFI debt with running a bargain basement staff. The current Government and key political stakeholders have resisted at all costs a national minimum staffing level, arguing primarily that this is not the overall number of nursing staff which matters but their suitability of skill sets in nursing environments.
These efficiency savings, nonetheless, have been made by NHS hospitals. Some hospitals have been more successful than others. The idiotic nature of the NHS drifting towards a market, being ensnared by the EU competition laws, that such financial assistance of hospitals come dangerously close to “state aid” which is deemed unlawful.
In England, “state aid” already exists in the form of foodbanks which have exploded in number under this Government. The consensus is that they have primarily supplied a need demanded from deserving members of the public, many of whom have been waiting for unreasonable time for benefits. This is a direct effect of the crass incompetence of operations in handling of benefits under this Government. This incompetence has seen emotional distress from people who are disabled. Some, it is alleged, have even taken their own lives.
The problem with running the country’s “safety net” in such a ‘lean matter’, means that there is no reserve in the system. If a nurse or Doctor goes off sick, the entire rota is thrown into chaos. The NHS ends up chasing its own tail, for example by employing expensive locum staff when it has not had the competence to employ the correct number of staff in the first place.
The mainstream political parties are still, overall, committed to the ‘private finance initiative’, although there have been some noises about how little value for money it represents. Despite the successful campaigning by some on the NHS, the political motivation for providing a solution to this problem appears lacking. There is an issue not only about the exorbitant demands of loan repayments, akin to a corporate ‘Wonga’ strangehold on the State’s finances, but also how private equity firms seemed to have got an amazingly good deal out of it effecting having a level of control and ownership on NHS hospitals which the general public, if they know, would balk it.
The next Labour Government is expected to introduce ‘whole person care’. Everyone agrees that social care is on its knees, but invariably most people agree that this situation has not come about suddenly in the last few years. There has been an insidious promotion of marketisation in the social care sector, which Labour had much to do with. Anyway, living in the now, the social care sector is in utter chaos. NHS hospitals are not able to discharge, often, their patients into social care in a timely fashion. Health and care sectors are intimately dependent on one other.
There is a growing feeling now that the drift in health and care policy across several governments, with a feeling of ungenerous funding, PFI, personal budgets, etc., albeit catapulted with the chaos over competitive tendering over the Health and Social Care Act (2012), has somehow resulted in an almighty mess. Like Lord Sugar, people are scrabbling around for a quick fix, but this is not going to be easy. Some of the strategies are clearly ‘science fiction’, unmarketable, or incapable of any teamwork. There appears to be too many Chiefs and not enough Indians. To coin the phrase by David Cameron, “We can’t go on like this?”
But in the meantime – the first management step must to be to say to Mr. Jeremy Hunt those immortal words…
“You’re fired”
We need to talk about the NHS
I’m essentially in two minds about whether the NHS is ‘a political football’.
On the one hand, I don’t think it should be.
I felt the way Mid Staffs meant some hardworking staff in that region came to be pilloried and demonised by the media was more than indecent.
On the other hand, I think you can clearly apportion blame for the current Government’s performance about A&E waiting times and other key metrics.
On balance, I’d like Labour to have a strong majority to get through repeal of the Health and Social Care Act (2012), without say relying on the Liberal Democrats who enacted it in the first place.
There’s also important legislative work to be done in bringing together health and care; and also an Act of parliament to consolidate regulation of clinical professionals.
While I have much sympathy for NHS campaigners, I most certainly do not want a weak Tory-led Government because of incessant criticism of Labour.
There is a huge amount to discuss about the NHS.
I believe, for example, that the private finance initiative, whilst it had a useful aim in improving the infrastructure of buildings of the NHS, clearly did not represent value for money.
I don’t think it’s ever justifiable to bring in the private sector because the NHS can’t ‘cope’. I don’t see why you should want to bring in locums either, because of ‘unforeseen circumstances’.
And, in total agreement with Jackie Ashley at a fringe meeting of the Fabians this year, there needs to be had somewhere a discussion of how health and care sectors are to be properly funded.
There is almost universal agreement that the NHS cannot function at anywhere near its best with social care in such chaos.
I do blame a supine media for not allowing discussion of ‘whole person care’, or discussion of topics that even Labour would like to talk about (such as PFI; see Margaret Hodge’s remarks).
We’ve got some brilliant brains involved – Prof Allyson Pollock, whose brilliant analysis of PFI shines, has had some very pertinent points about the Clive Efford Bill with Peter Broderick. Yes, Andy Burnham MP does not support ISPS/TTIP, but this policy is still being left hanging in an uncomfortable way.
I am fundamentally a socialist, so I take the perspective that if we’ve got money for war we’ve got money for the health service. And I think with debt going through the roof, and with the economy being fuelled with insufficient till receipts, we are a long way from the energy which saw the NHS created in the first place from the spirit of ’45.
Whilst supporting Labour, I don’t wish this to descend into tribalistic nonsense. I will support anyone who has decided that the current performance of the NHS is unacceptable, but I have no intention of actively campaigning against Labour.
I personally wish to see policy for living well with dementia progress under Labour, irrespective of whether Ed Miliband can eat a chip butty.
Whatever, we certainly need there to be a public discourse about the NHS more than Europe or immigration, for example. Socialism is social-ism; if you want to see how collectively we can pull through, just look at the energy generated by Jon Swindon (here) or Eoin Clarke (here).
The importance of the ‘lived experience’ at the Alzheimer’s Disease International conference in 2015
This year, the Alzheimer’s Disease International under Marc Wortmann has done outstanding work.
It is known for its huge impact in allowing nation states to flourish with dementia strategies
Its output is phenomenal (see for example this latest paper). I have no doubt whatsoever ADI will continue to flourish under Glenn Rees, the incoming Chair (currently Chair Elect).
I’m still very excited about the 30th International Conference of Alzheimer’s Disease International “Care, Cure and the Dementia Experience – A Global Challenge” 15-18 April, Perth, Australia, next year.
People who are very close to me will be there.
It is, also, a lovely city.
The conference website is here.
It was always emphasised that this conference would showcase the lived experiences of people with dementia. People living with dementia and caregivers were indeed encouraged to attend.
This is a part of the list of posters to be presented on Thursday 16 April 2014.
The two submitted by Chris Roberts and Truthful Kindness are shaded in a dark red.
The titles most clearly say ‘lived experience’ in the titles.
They were submitted as oral presentations, as the two people involved did not want them as poster presentations.
Indeed they did not opt for the ‘poster/oral’ option specifically for that reason.
P057
Communication with the world about my life’s experience with dementia after diagnosis
Truthful Kindness
Arts and Engagement
United Kingdom
P052
Living well with dementia: a lived experience
Chris Roberts
Arts and Engagement
United Kingdom
Truthful Kindness’ affiliation is Dementia Alliance International, Iowa; it was never submitted as United Kingdom. The irony about Truthful’s intended oral presentation is that she wished to explain how people with dementia can use all sorts of media to express themselves artistically and creatively. Arts and creativity is a huge policy plank in living well with dementia internationally.
It would have been clear to any diligent reviewer of these abstracts, from their submitted biographies, that both Chris and Truthful were genuinely living well with dementia.
Here’s Chris even holding the flyer of the Dementia Alliance International group, at Glasgow earlier this year in the Alzheimer’s Europe conference on dignity and autonomy in dementia.
Chris is currently a Board member of the Dementia Alliance International.
I understand, from having spoken to one of the juniors at the Alzheimer’s Disease International, that there may even be a chance for poster presenters to give short oral presentations of their work. But I think this possibly may be worse.
It has been explained to me that the environment for the poster sessions is very off putting. It is a crowded room, with not much space for the poster itself. It is a very noisy environment, which is very distracting. In other words, this can be an environment which is potentially disadvantageous to people with early dementia who wish to present.
I am, of course, pleased that the keynote speakers for this conference include two friends of mine, and whom I admire massively, and who are living well with dementia, Kate Swaffer and Helga Rohra.
As is known, I consider Kate to be exceptional in every way.
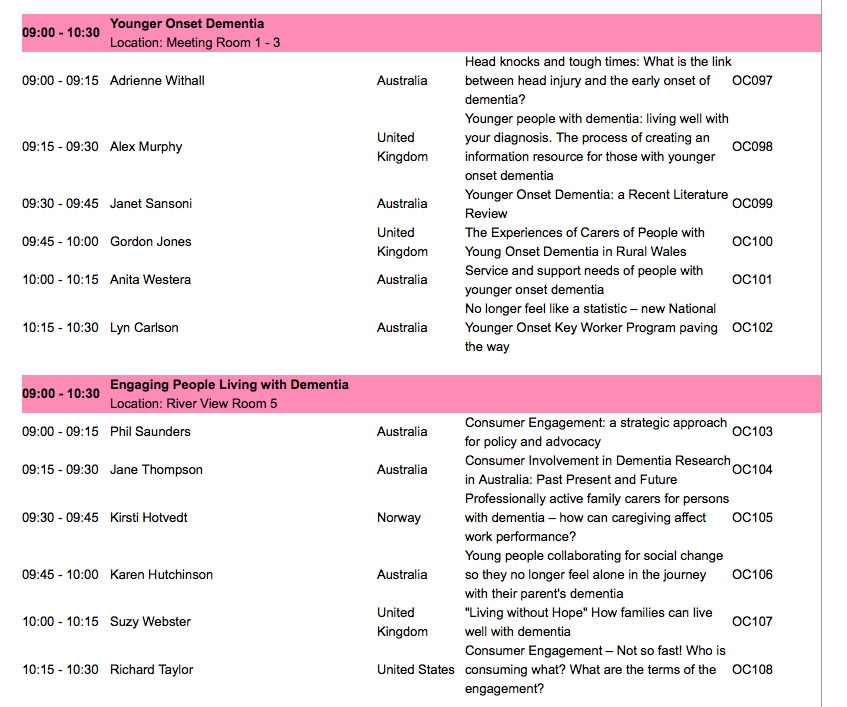
These are two symposia from the scientific programme in which they might have appeared: “younger onset dementia” and “engaging people living with dementia”. From eyeballing the titles of these talks, I don’t see many speakers talking about their own personal lived experiences.
The only parts of the conference yet to be revealed are the ‘workshops’.
The details of the workshops are given as follows:
Day 2 Dementia Friendly Communities
Day 2 “How to” topic to be confirmed
Day 3 Clinical trials
Day 3 “How to” topic to be confirmed
Day 3 Arts and dementia
Day 4 World Alzheimer’s month
Day 4 “How to” topic to be confirmed
I am extremely honoured to be on the international advisory board for the 2015 conference. I should therefore not want to criticise the organising committees in any way for their hard work.
But I cannot be a silent bystander to this either. The whole point about viewing dementia as a cognitive or behavioural disability secondary to a brain disease is that it then comes under international and domestic laws (for example, for UN Convention for people with disabilities and the Equality Act).
Ignoring two people’s wishes to have an oral presentation, as they cannot do poster presentations, is not making reasonable adjustments for their disability, one could easily argue.
I understand that the number of people with dementia fluctuates year on year, so it can be difficult to predict the number of people with dementia who wish to present. But, even with the limited number of places for the two symposia I have cited above, there doesn’t appear to me a big representation of people living well with dementia amongst the speakers, but I could be wrong. This also seems to be the case for other symposia, notably the one on “dementia friendly communities”?
I think the Alzheimer’s Disease International conference 2015 will turn out to be a brilliant opportunity for us to meet up; and we will also get a chance to discuss ‘cure’, ‘care’ and ‘living well’.
But Richard Taylor, living himself with a dementia, is right in his presentation from last year – where is the representation of evidence of psychosocial techniques?
I’d like to ask where is the evidence looking at ‘living well’, such as GPS trackers, design of wards, design of houses, the wider built environment, incontinence, eating well, assistive technology, ambient assisted living, advocacy, and so on?
On that note, I do strongly applaud the work of ‘Dementia Alliance International‘, which is truly representing the community of people living with dementia.
We hear words such as ‘challenge’ being used all the time in relation to dementia.
Hopefully the organisers will rise to the ‘challenge’ of living up to the reasonable expectations of those people with lived experiences wanting to take part fully in the ADI conference 2015 in a format they feel most comfortable with (and which makes reasonable adjustments if required).